Proudly Welcoming New Clients!

Welcome to Union Park Veterinary Hospital
At Union Park Veterinary Hospital, our primary goal is to treat your pet as part of our family. This means that the team at UPVH will treat your pets with the same state-of-the-art veterinary care and compassion that they provide for their own pets. Serving the communities of Cottonwood Heights, Midvale, Sandy, and the surrounding areas, the team at Union Park Veterinary Hospital are committed to your pet’s health.
Complete Veterinary Care in Cottonwood Heights, UT
We are a full-service veterinary hospital with cutting-edge medical equipment staffed by highly qualified veterinarians and support staff.
Thank you for making us one of the highest-rated veterinary hospitals in Cottonwood Heights, UT.
Your trust and support have been instrumental in our journey, and we want you to know how much it means to us. We look forward to continuing to provide you and your pet with only the best that the world of veterinary care has to offer.
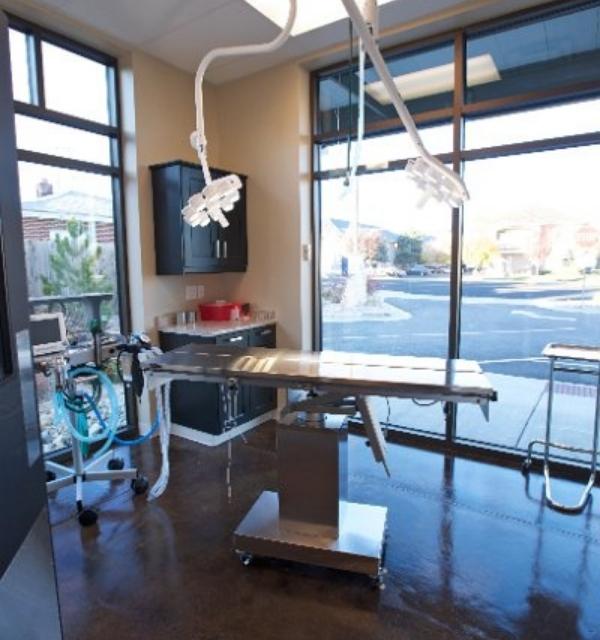
Look Inside Union Park Veterinary Hospital
We invite you to take a virtual tour and get to know our facilities, and we hope that you’ll decide to join us as a part of our extended family!